When Is It Necessary To Operate On A Herniated Disc?
Herniated disc is a common pathology that significantly affects the life of the person who suffers it. The option of operating on a herniated disc always arises when this situation has a great impact on the patient’s daily activities or if other types of approaches have failed.
Currently there are numerous techniques to operate on a herniated disc. Each is best suited to the characteristics of the injury and the patient, as well as the experience and preferences of the surgeon.
Thanks to this intervention, the quality of life may improve. However, it is not easy and it also involves a number of risks. In this article we explain everything you need to know about the subject.
What is a herniated disc?
To understand what a herniated disc is, you must first know the anatomy of the spine. The spine is made up of the vertebrae, which are individual bones. Between them are cartilaginous tissue discs whose function is to cushion the impact. They are the intervertebral discs.
Discs are made up of a nucleus pulposus and an annulus fibrosus. The annulus is the outermost part that surrounds the nucleus. As explained by specialists from the Mayo Clinic, a herniated disc occurs when the nucleus protrudes outward through a tear in the annulus fibrosus.
Hernias can occur anywhere in the spine. The disc can then irritate some nerves. Symptoms vary depending on the location and severity of the protrusion.
Herniated discs are very common. It is estimated that they affect between 5 and 20 of every 1000 adults under the age of 49. The most common is that they occur in the lumbar or cervical area and are accompanied by pain or alterations in mobility and sensitivity.
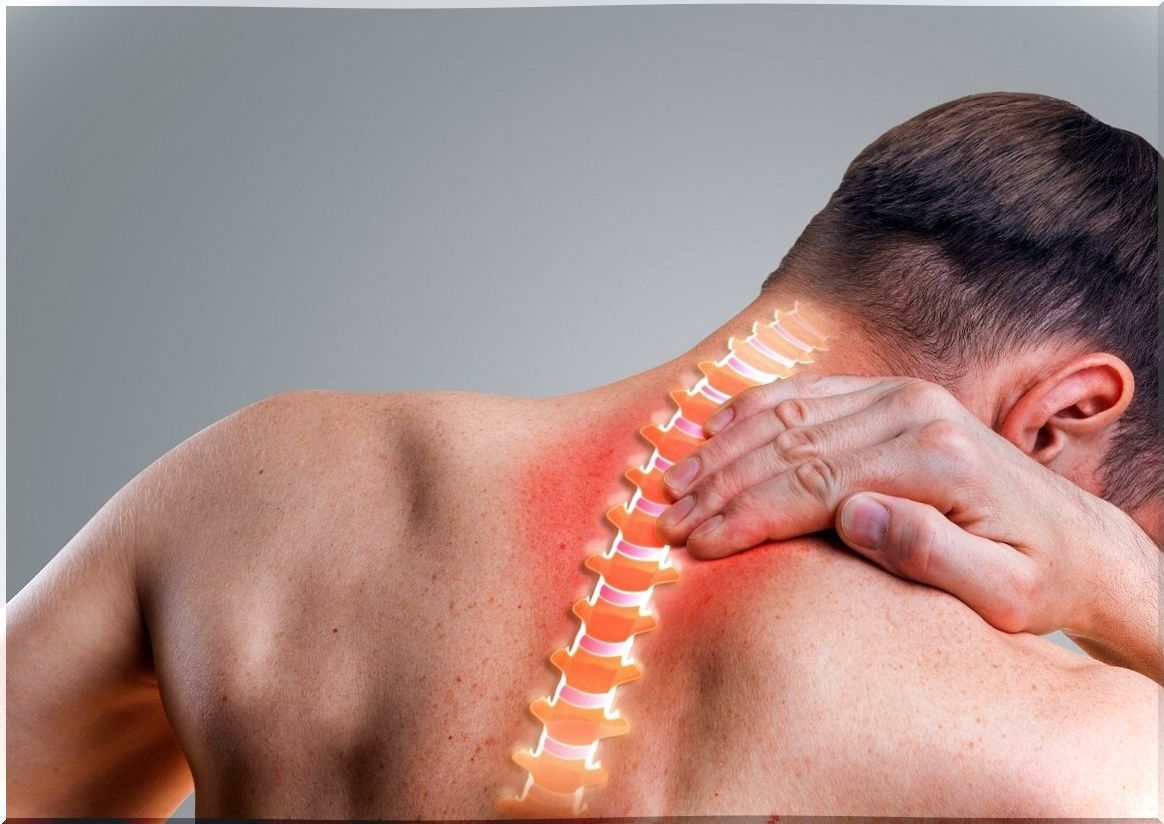
Herniated disc treatments
Before operating on a herniated disc, different less aggressive treatments are usually tried. The normal thing is to start with a pharmacological one to alleviate pain and discomfort. First, if the pain is mild, pain relievers such as ibuprofen or naproxen are recommended.
If pain control cannot be controlled with these types of drugs, corticosteroids can be tried. They are injected into the affected area, near the spinal nerves. In some cases, opioid medications are even prescribed.
The problem is that these drugs tend to create tolerance, dependence and addiction. In addition, they have multiple side effects. Therefore they must be used with caution. Any of the medical treatments is combined with physiotherapy and personalized exercises.
When is it necessary to operate on a herniated disc?
Operating a herniated disc becomes one of the options when the rest of the treatments have failed. The truth is that most patients do not require surgery. They tend to improve after days or weeks with the medical approach.
However, if the symptoms persist for months or there is disability, operating on a herniated disc is almost a priority. Disability can be a consequence of damage caused by the disc to a nerve. Mobility or the ability to control sphincters may be affected.
In addition, at present, there are different techniques to operate a herniated disc. In some cases, the intervention can be considered by a minimally invasive technique, with small incisions and a faster recovery. There are usually very good results.
Preparation to be able to operate on a herniated disc
To operate on a herniated disc it is important that the patient is aware of the risks and precautions prior to surgery. It is recommended that healthy habits are adopted.
For example, the ideal is for the patient to lose weight and get fit before surgery. Being overweight can put more strain on your spine than recommended. That is why the recovery process can be slowed down.
Strengthening the back muscles is recommended for any pathology that affects the spine. Exercises guided by a specialist should be performed to avoid aggravating the damage.
As with any other surgery, it is important to stop smoking. Tobacco increases the risk of surgical complications, in addition to interfering with the healing process.
What are the options to operate on a herniated disc?
As we have explained throughout the article, today there are numerous options to operate on a herniated disc. In the following sections we explain what the main techniques are and what they consist of.
Operate a herniated disc by discectomy
Discectomy is the most widely used technique to operate on a herniated disc. It consists of eliminating the damaged part of the disk or the entire disk. When the problem is in the cervical spine, it is done through an anterior approach.
In this case, a small incision is made in the front of the neck and the disc is removed. The space it leaves must be filled, replacing it with a small bone plug in most cases. An artificial disc can also be used.
Laminoplasty and laminectomy
Laminoplasty is a technique used to operate on a herniated disc in the neck. It consists of opening a space within the spinal canal, using a kind of hinge. The idea is to create more room for the herniated disc and thus relieve symptoms.
Laminectomy consists of trimming or removing a part of the vertebra that is affected. Thus, it is possible to expand the space in the spinal canal and reduce the pressure on the spinal cord, in addition to making more space for the nerves.
Cervical corpectomy
The cervical corpectomy is similar to the previous technique. It is a process by which a part of the vertebra is removed, but also of the adjacent intervertebral discs. An attempt is made to stabilize the spine using metal plates, screws, or bone grafts.
Spinal fusion
Spinal fusion is also a frequently used technique to operate on a herniated disc. It consists of joining the two vertebrae that contain the herniated disc. Many types of instruments can be used for this, as was the case in corpectomy.
Recovery from surgery
Herniated disc surgery has a relatively short recovery time. Most people go home the day after the procedure. However, it is important to avoid certain activities in the month after.
For example, doing very strenuous exercise or lifting heavy objects. Driving or sitting for very long periods of time is also not recommended. Squatting is also not beneficial for recovery.
However, a rehabilitation program may be indicated, which promotes faster recovery and improved mobility.

Risks and complications after operating a herniated disc
Operating a herniated disc is something that, in the vast majority of patients, is very favorable. The risk of complications is low and patients usually notice a marked increase in their quality of life.
However, that does not mean that there are no complications. For example, there may be infections or bleeding, especially in elderly patients. Postoperative fibrosis also appears, which interferes with the recovery of mobility.
The patient may not feel satisfied after surgery. It usually occurs in people in whom the damage prior to the operation was not well established. As there are no obvious signs that the symptoms were due to compression of a nerve, the signs are maintained and it is considered a surgical failure.
Herniated disc usually improves with medical treatment
Although operating on a herniated disc is a good option, the truth is that most patients do not require surgery. With medical treatment and therapy they usually improve markedly.
However, if the procedure is ultimately used, it is important that the patient is aware of all the risks and possible complications. However, there are usually good results and the quality of life of the patient improves.